A Comparison of Mental Health EHR Systems with Integrated Billing
For behavioral health clinicians evaluating practice management software
We have a theory about why so many therapists dread billing. It is not the math. It is the friction. The extra logins, the switching between systems, the rejected claim you discover three weeks after the session. Research consistently links administrative burden to clinician burnout, reduced patient time, and attrition from the field (Zhu & Eisenberg, 2024). When your EHR makes billing harder than it needs to be, it is not just an inconvenience. It is a practice sustainability issue.
What follows is an honest, contextual comparison of six widely used mental health EHR platforms and how they handle integrated billing. The kind of information you would get from a colleague who has actually used these systems.
Why Billing Integration Is Not a Minor Feature
Mental health professionals face administrative barriers across the entire practice continuum: credentialing delays, claims processing complexity, prior authorization, and denial management. For solo practitioners, who mostly lack dedicated billing support, that burden falls entirely on the clinician (Zhu & Eisenberg, 2024). Billing integration is not a feature to evaluate after you have picked your favorite interface. It is central to how sustainable your practice is.
When evaluating any platform, these capabilities matter most:
Superbill generation and customization
Direct insurance claim submission through a native clearinghouse
Automated ERA (Electronic Remittance Advice) posting
Out-of-network billing support
Client-facing payment tools and integrated credit card processing
Claim status tracking and denial management
My Best Practice: Billing That Thinks Like a Clinician
The platforms that work best for behavioral health billing are not the ones with the most features. They are the ones designed around how clinicians actually work. My Best Practice was built with that insight at its core: purpose-built for behavioral health, not adapted from a generalist platform.
From Session Note to Submitted Claim, Without Leaving the Platform
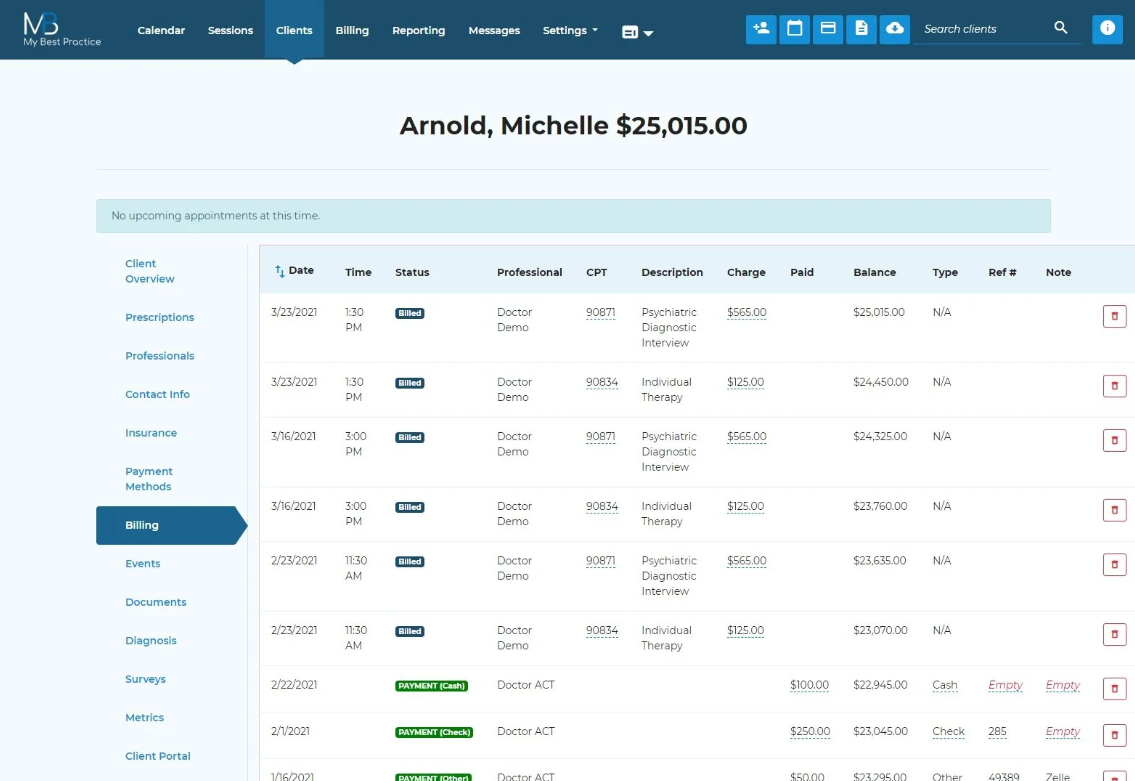
A clinician seeing 20 clients per week who saves just 10 minutes per session in billing time reclaims over three hours every week. My Best Practice achieves this by connecting steps that other platforms treat as separate modules. Completing a session note, generating a superbill, and submitting a claim are sequential actions within the same interface. No separate clearinghouse login. No re-entering data.
Through its integrated clearinghouse, clinicians can submit CMS-1500 claims, track claim status, receive and post ERAs automatically, and manage client balances in one place. For out-of-network practices, clients receive professionally formatted superbills with customizable billing codes and modifiers. When a claim is rejected, it is visible immediately, not discovered a month later.
Built for the Person Wearing Every Hat
Most behavioral health EHRs were designed for larger healthcare settings and then adapted. That origin shows in workflows that assume someone else is handling billing while you see patients. My Best Practice was designed around the opposite assumption: the person documenting the session is also the person submitting the claim. That single design choice shapes how every task is sequenced, and it makes a significant real-world difference.
TherapyNotes: Solid Infrastructure, With a Learning Curve
TherapyNotes has earned its loyal following. It is dependable, with a long track record in behavioral health, and its billing module covers the essentials: ERA posting, insurance claim submission, and client payment collection. The honest tradeoff is setup time. Clearinghouse integration is not plug-and-play, and claim status visibility is less immediate than in more tightly integrated systems. For solo clinicians handling their own billing without administrative support, that ramp-up period is worth weighing carefully before you commit.
SimplePractice: A Polished Platform With Some Billing Friction
SimplePractice is a well-known platform with a clean interface and a broad feature set. The billing experience, however, reflects its growth through acquisition and iteration. ERA posting and claim rejection management involve more manual steps than clinicians from more integrated systems may expect. Several billing features are also gated behind higher-tier pricing plans. For group practices with billing staff, the platform's breadth often outweighs these concerns. For solo clinicians managing billing independently, the tiered pricing and additional steps are worth factoring in from the start.
Three More Platforms Worth Knowing About
TheraNest (Now Ensora Mental Health)
TheraNest has a long track record and functional billing infrastructure covering insurance claims, ERA processing, and batch invoicing. The significant tradeoff is recent instability following its acquisition and rebrand, which affected platform reliability and support responsiveness. Pricing has also shifted to a per-provider model. Clinicians who depend on responsive support when claims go wrong should research the current state of the platform carefully.
Jane App
Jane App is frequently praised for its polished client-facing experience: scheduling, intake, and telehealth are consistent strengths. Its billing tradeoff is depth. Jane handles straightforward single-payer workflows adequately, but practitioners managing multi-payer environments, frequent rejections, or high submission volume often find the toolset insufficient. The platform's priorities are clearly oriented toward client experience, not billing power.
Healthie
Healthie is a modern platform originally built for nutrition and wellness providers, now expanding in behavioral health. Telehealth is strong and the interface is clean, but it was not built around the documentation and billing conventions of licensed mental health practice. CPT code workflows, therapy-specific note formats, and behavioral health payer requirements are secondary to its core design. For clinicians managing complex insurance billing as their primary revenue source, that wellness-first origin creates friction that purpose-built platforms avoid by design.
Before You Commit: Questions That Actually Matter
Feature lists are easy to skim and easy to misread. Run a realistic billing scenario during any trial period and ask:
How many clicks from session completion to submitted claim?
Is the clearinghouse integrated natively, or does it require a separate login?
Are ERAs posted automatically, or manually?
What happens when a claim is rejected, and how quickly are you notified?
Are superbills client-ready without additional formatting?
What billing support is available when something goes wrong?
The Bottom Line
Billing should not be an administrative project that follows every clinical day. For behavioral health clinicians who want integrated billing that does not require a separate billing specialist, My Best Practice delivers a workflow that is fast, comprehensible, and built specifically for how licensed clinicians practice. TherapyNotes and SimplePractice are capable platforms with large user bases, but both involve more billing overhead in solo and small-group contexts. For clinicians whose time is primarily allocated to clinical work, that overhead compounds quickly.
References
Zhu, J. M., & Eisenberg, M. (2024). Administrative frictions and the mental health workforce. JAMA Health Forum, 5(3), e240207. https://doi.org/10.1001/jamahealthforum.2024.0207
This content is intended for licensed behavioral health professionals evaluating practice management software.